Again, I’m sharing my experience with having active tuberculosis. Nothing I say should be construed as medical advice. Please speak with your doctor if you suspect that you have an infection. All of what I’m sharing is true to my own experience with TB so please do not take any of it as medical advice.
This is part 2, it turned out to be so long so I broke it into two parts. If you haven’t read part 1, yet, you should click or tap over to I had tuberculosis.
I will say, the entire stay at the hospital, I was in total denial. I didn’t believe that I had tuberculosis. I framed everything as in if I have it, if they know what my illness was. It was always an if.
I remember when they first came into that hospital room and told me, I said, “I need to call my pulmonologist.” I did call him before I left my first hospital room and begged his front office to put him on the phone because I was freaking out. He got on the phone and told me, “Well, I’m the one who called them. We sent samples from the bronchoscopy and the preliminary tests came back showing tuberculosis. I had to alert the hospital.”
My husband wanted to know more details and just wanted to figure out what we could do and what our next steps would be. He even tried calling to talk to my doctor, he had left a message but after a couple of hours of not hearing back, he actually drove over to his office.
I love my doctor because he’s hilarious without trying to be and his very matter of fact manner. He kept telling Curtis to calm down and that everything was going to be okay.
We were both so scared. In one way, it was reassuring to hear this and on the other hand, we didn’t feel like everything was going to be ok.
Side note: I had a routine visit scheduled this past December with my pulmonologist and he said you look good. You have come a long way. Before I left, he was standing next to me and gave me a side hug.
I texted Curtis afterwards and said my doctor hugged me! Gosh, I don't know if they know how I appreciate him and his staff so much.
While in the hospital, I was treated by an infectious disease specialist. He was a doctor who specialized in infectious diseases and especially had experience with tuberculosis. He told us that he used to work for the state working on their TB protocol.
He had a great bedside manner and spent a bunch of time with us answering our questions. I’m really grateful to him because he explained how tuberculosis is treated and how the patient is treated.
He told me that I was going to have to deal with the health department, that they would actually come over to my house and watch me take my medication. If I refused to take my medication, that I would be arrested and admitted to a hospital, probably one in south Florida, where they would force me to take my medication.
He mentioned the names of the medications I would be taking and he told me that I would be taking them for at least six months. He told me I was lucky because in the past it was up to a year on those medications! I can’t even imagine that! Even looking back, I can’t imagine that.
He explained that it’s a disease that is pretty old and there are laws in the books that say the government can make you take the medication for it.
Side Note: When this doctor found out that I wrote about food and photographed food for a living, he told me I had to try this Thai place near his office. He would rave about this place. We went that summer when I started to feel a little bit better and we loved it. I just ate there again yesterday with friends!
Frustrating times in the hospital
During my stay at the hospital, a couple of situations occurred that were really frustrating.
One morning, I woke up and my fever was back in full force. I wasn’t hallucinating, but I was starting to feel really delirious, and it made me feel really scared that I wasn’t going to get any better, that I was getting worse.
I was shivering and shivering, but then also sweating and not feeling really great. I also wasn't able to think straight. I remember one of the nurses came in and said, “I’m going to be back in five minutes with your medication,” and I remember looking at the clock and it was 7 A.M.
I fell asleep again because I was so delirious, and I woke up again at 10 A.M., and there was my nurse with the medication. She gave me my Tylenol and within a half an hour, my fever broke and I was feeling so much better. That’s when I started feeling really angry because I should’ve had my medication three hours before. It was so frustrating and it made me think of people who are much sicker than I am in hospitals all over.
What I learned: You have to be firm but nice. Even if you have to ask for something over and over again, do it. Be persistent. Keep track of your medications yourself and when your last dose was and when your next dose is supposed to be. Be your own advocate and if you can’t be (because you’re sick and it’s hard to be your own during that time), you need someone who you love and trust to be pushy for you.
The first night in the isolation room, they brought me the medication to treat tuberculosis. No explanation of the medications or what they were. They said, here take this. It was four different medications and a vitamin.
They were:
Rifampin
Ethambutol
Isoniazid
Pyrazinamide
Pyridoxine
A couple hours after my first dose, the nurse came back to check on me. I had just gone to the bathroom and I was freaking out because the toilet bowl was orange and I probably shouted, “Something’s wrong! I think I’m bleeding.”
I mean it was dark, so I couldn’t tell that it was orange, it looked red or purple to me. The nurse asked me, “Are you on your period?” and I looked at the nurse thinking, “Okay, I’m a grown woman. I think I’d know if I was on my period.” It was just laughable that she would ask me that.
The next day, one of the respiratory therapists told me I could request the names of the medications and the information sheets on them. So I did and when they brought the sheets in, the respiratory therapist reviewed them with me.
It turned out that Rifampin actually turns your bodily fluids orange. That was a fun experience especially since I had to take it for six months. (That's sarcasm! LOL There needs to be an emoji for sarcasm…)
Every few hours, a nursing assistant checked my vitals and each day they drew blood to run tests and also listened to my chest. Some of the doctors and nurses could hear a crackling noise in my chest, some of them said they didn’t hear anything and that I sounded fine. LOL
I could hear a creepy creaking noise in my chest. Sometimes I would hold my breath to see if it would stop but it didn’t. I kid you not, it sounded like creaky stairs in my chest and someone was walking on those stairs making them creak.
I had friends visit me in the hospital. Everyone that entered the room had to wear a mask and gown. I felt grateful they wanted to go to all that hassle to visit me in the hospital. And I couldn’t help but get emotional every time someone visited me.
I was still in denial it was TB. I felt vulnerable and tired. My family wanted to visit but my closest family lives over an hour away. I didn’t want to burden them with having them come to visit.
My Mom was sick with a cold (I think) at the time and I didn’t think it was a good time for her to visit. And I felt guilty and worried that I might have exposed any of my family and friends that I had been around during the last few months.
At a certain point, I began to feel better and asked to be taken off of the pain medication because it was an opioid. So that’s when they switched me back to Tylenol for my fever.
My attending physician mentioned to me that once I didn’t have a fever for 36-48 hours straight, I could go home. On Saturday afternoon (day 3), I was feeling much better. I had asked them to unplug me from the IV machine and cover my arm so that I could take a shower (which they had done every time I needed to shower).
When I got out of the shower I had decided that I was going to put on pajama pants and a t-shirt instead of the hospital gown. I was feeling much better, and I sat there for a few hours and no one came back to plug me back into the IV machine.
I wanted to go home
At that point, for a couple of days now, I had been taking oral antibiotics, so the only thing that was coming through the IV was saline water. I was talking to the respiratory therapist and I said, “I don’t really think I need this IV anymore,” and she said to me, “Well, you can ask them to take it out.” I said, “I can?” and she said, “Yeah, you can refuse it.”
That’s when I decided to call the nurse. When she arrived, I asked her to remove my IV. She was insistent that I shouldn’t do this and said, “We advise against this, we don’t really want you to take it out, we think you should keep it in in case something else happens.”
I could tell my respiratory therapist wasn’t looking at me, she didn’t want me to shout out to the nurse that she had told me I could refuse the IV. No way was I going to do that.
You don’t do that. I don’t know how many times I have said this but you don’t sell out someone who is helping you. (Of course, as long as they aren’t harming someone else or doing something illegal.)
I told the nurse, “Well, I refuse this and I want you to remove the IV.” The nurse came over and pretty much yanked it out of my arm (it really hurt when she did it) and told me to put my hand over it. Then, she left.
We were sitting there for a little while and she looked down at my arm and said, “You’re still bleeding. She didn’t bandage your arm?” I said no, “she had told me to place my fingers on my arm and never came back to bandage my arm.”
That’s when my respiratory therapist started looking at a first aid box (or was it a supply box?) that was in my hospital room and there were no bandages or gauze. She then left the room, having to go through the whole procedure and again once she returned with a bandage for my arm.
One night during my stay, I couldn’t sleep because another patient down the hall wouldn’t stop yelling and screaming. When my nurse entered my room, I asked about the yelling. She told me they were ignoring him.
They won’t let me leave the hospital
At this point, I had started asking the nurses who came into my room if I could see a doctor to discharge me. The response, “Well, your doctor’s not here, your doctor’s off for the weekend.”
Being persistent, I kept calling the nurses’ station. At one point I said, “I’d like to speak to the head nurse,” and they responded with, “We’re trying to get your doctor to approve it.”
Then, at one point, the head nurse actually came into my room and said, “We can’t let you go. No one will discharge you, no one is here.” Basically, the answer I got was that they’re short-staffed on the weekends and they don’t really do discharges on the weekends.
They told me that the physician treating me wanted to confirm with the infectious disease specialist my prescriptions before discharging me.
It just boggled my mind, I was sitting there in my pajama pants, no IV in my arm, and watching T.V., and I felt like I was in a really overpriced hotel room at this point. I just was really frustrated and wanted to leave. I felt so stir crazy because I couldn’t leave that room.
Side note: I watched the Cinderella (live action) movie on tv in my hospital room, it was my first time watching that movie. I bawled when Cinderella’s mom told her to have courage and be kind. It sounds so cheesy but I felt like her character was speaking directly to me.
Curtis would come visit me and stay with me for the whole day but like I mentioned earlier he had to go home at night and take care of the pets. He would spend a lot of time looking out the window and say, “You have a really nice view.” I responded by saying, “I don’t care.”
To this day, I can’t even tell you what it looked like out there because I didn’t even want to look out the window. I wasn’t allowed to leave the room so I was frustrated.
The next morning (which was Sunday), I saw my doctor and he said, “I’m really sorry you couldn’t leave yesterday, we had to get your medications straight.” They gave me prescriptions for the five medications and I was able to go home.
That afternoon, on the way home, a dear friend of mine texted me asking how I was and if I had received the flowers she and a couple of other friends had sent me. She had paid for them to be delivered to my hospital room.
I told her that, “No, I didn’t get any flowers.” She responded by saying that she would reach out to the florist the next day (Monday).
She spoke to the florist and the florist even called me. The flowers were delivered by her husband on Saturday afternoon. They left it at the nurses’ station but I never received them. She sent him back to the hospital on Monday. The nurse who signed for them told him I don’t know what happened to them, I think they were delivered to the patient.
He then went outside and called his wife and she told him to march back in there and tell her she would need to pay for the flowers since they were never delivered to the patient. He suggested to his wife to put together a new bouquet so he could deliver it to me at home. She said no way, you need to go back in there.
He went back inside and told the nurse what his wife told him to say. They scurried around looking for the flowers and turns out it was in a linen closet. We all wondered how they got there. He delivered them to my house and I was so grateful.
Kindness and Thoughtfulness Matters
At first, I thought it best to not make a big stink about this…but then when you think about it, my dear friends had taken the time to send me beautiful flowers because they were thinking about me. They wanted me to know that I was loved and that they cared.
When someone has a serious illness, these tokens of love and thoughtfulness mean so much. They really do. Especially at a really vulnerable time and you’re not feeling your best.
It’s hard to not think that the flowers were purposefully not delivered to my room because I was being persistent about getting discharged.
While I was in the hospital, I did google tuberculosis on my phone. Most of the sites that popped up were about TB symptoms and treatment. I only found a couple of firsthand accounts. They were aid workers who got sick in faraway countries and came home to the U.S. to be treated. One of them had to be quarantined for months and she became depressed. The other case was so serious that she had to have parts of her lungs removed.
There were times in the hospital where I was really scared. I had moments where I wondered if I was going to die. So when my friends thought of me and ordered flowers and whoever at the hospital decided they weren’t going to take the time to deliver them to me, it just pissed me off.
But more than that, it upset me. If it could happen to me, it could happen to others.
Curtis took me home from the hospital when I was discharged and then went to the pharmacy to fill the prescriptions. The pharmacy only had 4 of the 5 medications. I later found out that a month (or two?) supply of these meds costs upwards of $2000.
We were lucky to have good insurance at the time and paid a total of $200 in copays for the meds they did have. I took the medications that night and Curtis went to a different location to pick up the fifth one.
The health department calls me
On Monday morning I received a phone call from a gentleman who works for my county’s health department. He told me that he had in front of him results from the state’s TB lab. He told me that I, in fact, had TB and that the hospital should have called the health department.
And that he would have seen me in the hospital. The entire time, he was just shocked that the hospital didn’t call him. Then, he told me that the health department would be handling the medications, they would be bringing the medications to me, and, just like the infectious disease specialist told me in the hospital, that they would deliver my medications and watch me take them.
He told me to throw away the $2,000 worth of medicine we had just bought the day before. He told me that I couldn’t use it as they are supposed to dispense the meds directly. I was so grateful that we had insurance and that we hadn’t just shelled out $2,000 for medicine you can't return.
But $200 is still $200 and we wouldn’t have spent the money and wasted these medications if the hospital had called the health department like they were supposed to. I wouldn’t have received those prescriptions if they had called. And maybe I could have left the hospital a day earlier.
One of the things I learned on the call was I was to be quarantined for two weeks. I needed to stay home and stay away from people with compromised immune systems, children and babies. When I was in the hospital, they asked me over and over again if I had children. Now I knew why.
He told me I could take walks but that I should generally stay home. They understood that I would have follow-up appointments with doctors so during the quarantine period, I would need to wear a mask when I went to a doctor’s office. But the main thing was I should avoid areas or rooms that are not well-ventilated.
I remember framing everything again with an if. If I had tuberculosis, if the final tests come back as TB, were we sure that I had tuberculosis? I was told in the hospital that I would take eight weeks for a full culture to come back with a definitive result of positive for active tuberculosis.
That made me think, there’s a chance I don’t have it! But looking back, I know that didn’t make sense, my hoping it wasn’t TB. Which meant I was hoping they were wrong and didn’t know why I was sick. Because active tuberculosis is highly contagious, they don’t wait the 8 weeks to find out. If initial tests come back as a possible positive, they make you take all of the medications to treat you for TB.
I asked what percentage he was certain that I had tuberculosis. He told me 97%, that he was 97% sure that I had TB.
I had to do a series of tests. I had to give the health department regular sputum samples. I’m sorry if this sounds gross. I had to inhale deeply and try to cough from the bottom of my lungs and then spit into a cup.
Once I had a couple of consecutive negative tests, the quarantine would be lifted, which meant that I was no longer contagious.
Why health departments are tasked to watch TB patients to take their medicine
The reason health departments are on TB patients to take their medicine, they shared with me, because once they are not contagious and when they start to feel better, in the past, they would stop taking their medications. Which is bad news since you’re taking antibiotics. This would create a resistance to antibiotics.
During the time I was quarantined, I talked to my therapist over the phone and did our sessions that way. I’m grateful to her and having the ability to talk to a third party about what I was going through. It helped me process it which looking back was a saving grace.
Every day, except the weekends, they came over and gave me my medication. (On Fridays, they would give me enough medication for the weekends for me to take on my own.)
At first, I was taking 10 pills a day. But at the two week mark, I was allowed to opt into taking 21 pills twice a week instead of the 10 pills a day.
The nurses at the health department were always nice. When they came over, we would sit on my couch and chat while I was taking the medicine. They would ask me how my day was going, answer any of my questions and chat with me like they were my friends. But I know their sole purpose in coming over was to deliver my medications and watch me take them.
The medicine made me so sick. Actually, I get emotional thinking about that time because I could barely eat and I could barely do anything. It just made me feel overall ughhh. I spent a lot of time on my couch. When I could, I would watch Netflix. I rewatched every West Wing season (the best TV ever), I watched the Newsroom for the first time and I even watched all of the episodes of the OC.
I went to see both my primary care doctor and the infectious disease specialist as a follow up to the hospital stay. One of my doctors told me that basically, I was going through a chemotherapy treatment. It was four very strong antibiotics and a vitamin (because one of the antibiotics strips your body of vitamin B6).
I remember my primary physician telling me that I needed to let my body heal and I needed to be gentle with myself. I was getting so frustrated that I couldn’t work and I was getting frustrated with my body. Through it all, she was very nice and I remember that day I was bawling in her office, she gave me a hug.
I even had a nice chat with her after the whole chest x-ray fiasco before I ended up in the hospital. Something happened with my chart and it never made it to her desk to call me with the radiology report. She took full responsibility for it and even apologized.
She even gave me her cell phone number for whenever I needed it. I remember texting her the night I was in the ER…asking her what I should do. She did respond and told me that I should let the hospital admit me and figure out what was going on.
Back to the meds, they made me really sick. Since I was on twice weekly, the medications made me feel sick for a couple of days. When I would start to feel a little bit better, it would be time to take the next dose.
I opted for Mondays and Thursdays and pushed them to come as late as possible in the afternoons. Having them come in the afternoons left me with two mornings a week where I would feel a little bit better and I would try to get some work done.
One of the other milestones I was waiting for was to see if the strain of mycobacterium tuberculosis that I had was antibiotic resistant or not. They told me once that test came back as negative, I would be able to remove one of the medications.
In total, I was unable to work for four months that year. Early on after I came home from the hospital, I had an impending deadline for a client. This client was understanding and kept telling me that it was ok and I could take my time. I was really late turning in my work but they were accommodating. They have no idea how much it meant to me that they were flexible and understood that I was really, really sick.
One of the regular things I had to do besides taking the medications was to get regular bloodwork done. One of the medications can affect your liver and they wanted to track that.
I had to get an HIV test
When I first talked to the health department, they told me they needed to test me for HIV. If I was HIV+ then the treatment for TB would be different. I assumed I wasn't HIV+ but the anticipation waiting for the test results was not fun.
A couple of weeks went by and they didn’t mention the HIV test results. I was in close contact with the health department, talking to them several times a week. So I finally asked about it and they told me that the lab complained they couldn’t run the test because there wasn’t enough blood in the vial.
It was frustrating dealing with the health department
So I returned and a different person from the health department took my blood sample. She asked me which arm she should use. I told her my left arm. One of the things I do when I have to take a blood test is I don’t look at the needle, I just make sure they’re wearing gloves and then I look away.
At one point, she mentioned that there was no blood coming out. And the vein had collapsed. I looked down and she had actually stuck the needle into the same vein as where my IV was from the hospital was placed, and that vein had not healed yet. That arm was looking really gross. I told her this and she said let’s try your other arm.
She had to stick me three times to actually draw blood. It was excruciating. I never had a problem with blood draws until that year probably because I had to have blood drawn so many times. It’s hard for me to get blood drawn today. I wiggle around and I try not to get anxious but it’s hard not to!
So of course, after that, I talked to my primary care doctor and she wrote me a standing order for all of the blood work that the health department needed and some extra tests. It was great, because then I can pick where to go to get my blood work done. I went to the place I usually go to, the lab I mentioned earlier. It doesn’t hurt when they do the blood draws.
Same thing with my x-rays and my CT scan when I had to get another one done. My pulmonologist did the order. I used my health insurance to help pay for these tests. I could have done it through the health department and it would have been covered by my county or my state but doing it through my insurance I could pick where I wanted to go and not have to deal with some of the ridiculousness.
Side note: During that time, I found out that I’m vitamin D deficient. Like dangerously deficient. I take a prescription supplement every other week now and it helps my energy level tremendously and I don’t get weird muscle cramps anymore!
Over time, I realized that I needed to stop questioning whether I had TB or not. Even if I didn’t fully believe in this diagnosis, I was starting to feel better. I was coughing less and less.
Not that I was trying to deceive them but I knew I needed them to know that I would be in compliance. I was taking my medicine and actually in the end, never missed a dose the entire six months I was being treated.
I was given another patient’s medications
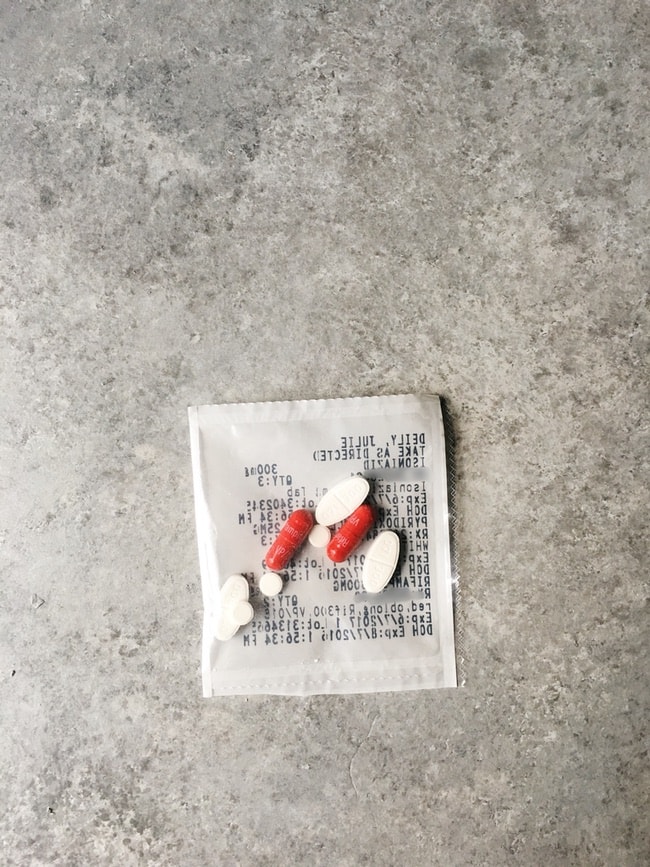
I think it was May, a Monday or a Thursday, one of the nurses arrived from the health department to give me my medicine. After a month or two of getting meds from them in an orange bottle with my name handwritten on it, they started bringing my medication over in a little plastic bag that had my name, birth date and medications and dosing printed on it.
You tear it open and just take the medication. I know you have seen ads for this service on TV and on social media. I have!
I have a placemat on my coffee table and I always sat in the same spot on the couch when they came over. They always sat across from me and would have a casual conversation which was always disconcerting because I know they were watching me to make sure I took my medicine.
I always tore open the packet and would let the pills drop onto the placemat. Some of the pills were pretty big so I would take them one at a time. When I was taking 21 pills, it felt like it was going to take forever to finish them all. (Over time, when I would hit certain milestones or time periods and they would remove a medication or lessen the number of pills. Towards the end, I was taking 8 pills twice a week.)
I would always hold the little plastic packet with my name on it and play with it with my fingers, moving it up and down and twirling it. That was just a nervous tick I had.
At one point, it didn’t seem to register fast enough in my brain for me to spit it out. I had realized this wasn’t my pill packet. It had someone else’s name on it. And then it registered and I could blurt out, “These aren’t my pills!”
She said, “What?” I replied saying my name isn’t on there, there’s someone else’s name on this pill packet.
She had no idea how it happened and was flummoxed. She probably shouldn’t have told me this but she mentioned that this other person was double my size and had more pills in his packets than I do.
She looked at the pills that were left on the table and calculated in her head the ones I had already taken. And she said with confidence (although I don’t know if I believed her) that I had only taken what was prescribed to me and what was left on the table were the pills I didn’t need or shouldn’t take.
I was pretty gobsmacked that I was given someone else’s medications. My level of frustration with dealing with the health department only grew. Again, they were very nice people but I was still frustrated.
In June, I kept asking them for the final culture results. I knew the 8-week mark was coming up. Every time I saw them or talked to them on the phone, I asked them for the results. It was probably annoying them because every chance I got, I asked them if they received the results yet.
I’m talking about that original sample that was taken out of my lungs by my pulmonologist. The state lab had cultured it and I was waiting for that final result.
Finally, I got the results, they handed me the paper that said Julie has TB. Not exactly that way but you know what I mean. This was weeks after the 8-week mark, by the way. The date on results was dated three weeks earlier. To say that I was mad was an understatement. But what could I do?
Towards the end of June, it was nearing the halfway point for my six months of treatment for TB. So I started asking, what is the date of my last dose? I wanted to know so I could put it in my google calendar! I love looking forward to a certain date. I get to count down, I guess you could say.
They kept giving me the runaround. They kept telling me it depends on different variables and what if I missed a dose? I told them, I haven’t missed a dose yet and I don’t plan on it. All of the nurses kept avoiding the question when I asked about the date of my last dose.
So finally, one afternoon, the nurse who had accidentally given me the wrong meds called to ask about what time she could come over with my medication. I told her that I have been asking for my end date. She started telling me the same thing that everyone else said.
I finally said, “You know, honestly, I’m not a child. I totally get that things could change, but I just kind of want the date and I’m really frustrated because I had asked for that final culture for weeks, and then I finally get it, and the date on the report was three weeks earlier.
The other thing is, the other day you came over with someone else’s medication, I never told your boss about that. So, I just really want a date. Just give me an end date, I know it might change.”
She responded by saying, “Okay, let me see what I can do.” She gets off the phone and her boss calls me back ten minutes later. He says, “Okay, here’s the date, it might change,” and I said, “I know, I just want to put it down in my calendar.” When I counted how many doses, it wasn’t the exact date that I thought, but it felt good to me to have this final date. I thought to myself, okay, this is when I’m going to start feeling better.
June was a big month, I started traveling again. I went to Boston for a blogger retreat and it was so fun to be among friends and “co-workers” again. I started to feel like I was coming back to the land of the living.
Because I hadn’t missed a dose meaning I was compliant, the health department was able to give me a cell phone that had wireless service. The only thing you could do on the phone was take a video of yourself taking the medicine and upload it to a server that my health department had access to.
I had to take a selfie video showing them the pill packet with my name on it and showing them each pill in the camera as I took it. This was great because I didn’t have to meet them twice a week in my living room anymore. And I could take the medication as late as I could which meant I could actually eat dinner!
Side note: another reason why I love technology!
For a long while, I don’t remember exactly how long, I slept in the guest bedroom. I didn’t want to get Curtis sick. I felt a huge amount of guilt because the initial blood test showed Curtis had been exposed to TB. They ordered a chest x-ray and didn’t see any TB infection in his lungs via the x-ray so they gave him the all clear.
I was told that consistent and close contact with a person with active tuberculosis (who is contagious) is how someone else could “catch it”. My mom and a couple of siblings who live closest to me were tested and they all came back negative. But it wasn’t a surprise to anyone when Curtis tested positive for TB exposure.
He’s my spouse and we share a bed together so while I was contagious, he had close and consistent contact with me. Again, I’m so grateful that he never got sick.
I’m so glad he didn’t have to be quarantined and miss work for 2+ weeks. But because he was exposed, he had to take Rifampin for 4 months. I felt terrible because that’s the medication that turns stuff orange. I know. Ugh
Aside from the medications wearing me out, a lot of the time I felt too sick to eat. I had a nauseous feeling in the pit of my stomach for most the time I was on the medications. And one of the medications caused joint pain. The joint pain thankfully stopped a few months after I finished the medications.
I finished my tuberculosis treatment in October 2016. I had another chest x-ray ordered by my pulmonologist that December and it showed my lungs were healing.
I was told by the health department that I would probably have scarring in my lungs and if someone was trained to see it, they would be able to see the scarring in my lungs (and know it was from TB) via x-ray.
I was diagnosed with an immune deficiency
In December 2016, my allergist (who is also an immunologist) diagnosed me with Mannose-binding lectin deficiency. Finally, I had an answer. All along, everyone said I didn’t fit the profile of someone who could have active tuberculosis. That it didn’t make sense. That something in my history had to account for why I was not able to fight off the dormant TB any longer in 2016.
I kept asking my doctors for answers on what my something was. What was that something? My doctor ran a battery of blood tests and discovered the deficiency. He told me that a lot of doctors don’t know about this deficiency so they wouldn’t be likely to run this test.
It just means that I have a deficiency of an immune system protein. I’m more susceptible to upper respiratory tract infections. I’m more susceptible to pneumonia and meningitis. Likely caused by a genetic mutation, I was told there’s nothing they can do about it.
There was something I could do though, I was advised to get both pneumonia vaccines as well as the one for meningitis. Over the last couple of years, I have gotten all three of them.
It took over two years for my body to heal after I completed the medications but even after being given the all clear from the health department, I had what seemed like an unshakable anxiety about getting sick. About being around sick people.
I could feel the anxiety materialize when I heard someone near me have a coughing fit. I was constantly worried that I would get sick.
Because when I get bronchitis, it always takes me longer to get better than anyone else around me. And I got it pretty much every year. So the immune deficiency diagnosis made so much sense. As a child, I was sick a lot.
Every few months, I would feel more of my energy level coming back. I would think I’m all better now. I’m ready for whatever comes next and then a few months later, I would feel even more energized.
I realized that my body had to heal and I had to give it the time and space to do so. But during that time, I wanted to rush it. I was tired of being sick and tired of being tired.
Where I’m at today
If you have stuck with me this long, thank you…I know these posts are so longgggg.
Today, I try really hard to listen to my body. Sometimes, I’m not very good at listening to it but I am better about it than I was 3+ years ago. I really try hard to rest and drink a lot of water. I don’t share food or drinks with anyone.
I try to do yoga regularly and I try to keep my stress level down.
A couple of the most important lessons I learned was that you quickly find out who your real friends are and what truly matters.
What matters most to me are my friends who care so deeply, friends who want what’s best for me and who support me. What matters to me is that I live authentically and only share with you the things that I love but at the same time, share with you what's going on and being real.
It’s interesting how there were little things that used to bother me before my illness and I could give a crap about those things now. And there were things that I didn’t prioritize but I prioritize them now.
From the friends who had flowers delivered to the hospital and the ones who showed up in my hospital room and wore a mask and sat and chatted with me. Even though, I didn’t know what to say and couldn’t stop crying because I was so scared.
And the friends who sent us a gift card for groceries. And to the friends who sent us food, even though I couldn’t enjoy it in the moment, it mattered and I appreciate them for it.
I remember telling one of my sisters years ago, we have been through so much. We can get through this. I tried to channel that feeling and those words even in my darkest times during my illness. And there were dark times.
For a long time, I really wanted things to go back to the way they were. But I know now that it’s not possible.
Now I try to take time and pay attention to what I need first. Which means staying hydrated and getting enough sleep. And that means saying no more often than I did in the past. Saying no more means I will have energy for the things that are most important to me.
In November 2016, I talked to my doctor about this constant neck and back pain I was having. After an MRI showed I had a herniated disc in my neck and several bulging discs, I realized I have to work even harder on lessening my stress even more. Even not getting enough sleep, causes muscle spasms in my neck and back.
Everything has changed and I can’t go back. I learned so much from this experience, about myself and about others. And today, I can honestly say I wouldn’t change a thing.
Everything has changed and yet, I am more me than I’ve ever been. –Iain Thomas
The last lesson that I learned and wanted to share with you is to always ask for copies of test results, reports and imaging. Today, I always ask for ultrasounds, x-rays, scans on a disk so I can keep and if needed, I can take to another doctor. Sometimes, doctors and nurses are taken aback because they are not used to patients asking for copies of everything, even a negative test result. But I tell them, it’s a habit I have developed after having active tuberculosis.















Suzanne M. says
Thank you so much for sharing your experience. It’s shocking how many times the system failed, and it makes me wonder what happens to people who aren’t as able to check/follow up/advocate as you were doing. I am glad you are doing well now and recognizing what you need to stay healthy. All the best!!!
Mary Swain Landreth says
I agree it is important to share your story and brave of you to do it. Wonderful that you are practicing such good self care and have loving and supportive friends and family. I am sure your story will encourage others to have an advocate to ask all the questions and insist on good and prompt care for their loved ones. You have given people a gift! Thank you.
Karen T says
I am so sorry you had to go through this awful journey. You are a true warrior and an inspiration. I am so sorry it took so long to get an accuarate diagnosis and you are absolutely correct that everyone who is sick in the hospital needs an advocate. The fact you made it through this and feel you came through it more you than ever is such a positive way to process this entire, long, arduous ordeal. I am grateful you are better and feeling stronger. Listening to your body is so vital to your health and you have mastered it. Best regards for continued good health and thank you for sharing your illness and climb back to health with your readers.
Laurel Jenner says
Julie, we need to talk! I also had TB, but took those horrible drugs for 12 months. It was a very difficult year, those drugs were so hard on my body. Many years later I was also diagnosed with primary immune deficiency, specifically CVID. I’m being treated with weekly blood plasma infusions. My immune system comes from healthy people’s blood plasma donations.
The health department tested everyone I worked with, went to school with, friends, etc. everyone was negative, thankfully. I have 3 children, they were tested every year for the first 10 years of their lives.
I also have nightmare stories about all the doctors, hospitalizations, terrible communication, etc.
You are not alone. I think if we got together, we’d end up laughing together at the ineptitude of the professionals ment to care for us.
Jen says
I am so sorry you went through such a horrible ordeal especially when you feel so terrible. ???? Thank you for sharing your story.
Shari Sweeney says
As an old (old enough to be your grandmother) Chinese/Hawaiian woman I was riveted by your account. And horrified. I’m so glad you made it through but I feel you were treated terribly by a number of people and that you encountered a great deal of racism.
In this time of Covid and Black Lives Matter your story though different had similarities of many. I am so glad you showed and shared your strength and fortitude and pushed through to the other side. Thank you for sharing.
CATHERINE Pasquinucci says
Bless your beautiful heart and soul❤
Julie Deily says
Thank you for your kindness!
Elise Bauer says
Oh Julie, what a tremendous ordeal you’ve been through. Thank you so much for sharing your story with us. I’m so sorry you have had to put up with so many indignities and your health care providers not communicating well with you. And another person’s meds??? WTH?? There are protocols for preventing these kinds of mistakes and it’s clear that these protocols were not being followed. I’m so thankful that you made it to the other side of this. xoxo
Julie Deily says
Thank you, Elise. I’m so thankful as well. I appreciate your friendship so much!
Lynda says
Wow! I am so shocked at how poorly our health care system treated you. So. Many. Things. went wrong in your situation. That was awful and I am sorry that you went through it. Thanks for sharing your story so that others can be proactive about taking charge of their healthcare.
Julie Deily says
Thank you, Lynda, for your kind words!